
- Home
- >Health professionals
- >Breast screen process and breast density
Breast screen process and breast density
Breast density
BreastScreen NSW will commence reporting mammographic (breast) density at the end of April 2025. We will use software to report density to clients and their nominated GP.
Scroll down to find out more about breast density, including:
Your recommendation is important
Women are more likely to have a breast screen (mammogram) if it’s recommended by their doctor.1520
A referral is not required, however our request pads are available to order.
Maximising participation in screening
Only half of all women aged 50–74 have regular screening mammograms with BreastScreen NSW. Here are some concerns women may have towards screening.
The health advantages of getting a breast screen far outweighs any concerns. We encourage health professionals to talk to women about the benefits of breast screening.
Learn how to increase screening participation rates at your practice. Visit the Primary Care Quality Improvement Toolkit.
Breast screening guide for health professionals

- Women aged 50 to 74 are invited every two years.
- Aboriginal and Torres Strait Islander women are recommended to screen from 40 years.
- For women aged over 74, it is recommended that GPs discuss with patients whether routine breast screening is a health priority.
- Find more information on:
* Symptomatic women should be referred to diagnostic breast imaging and/or a breast surgeon. Screening mammography alone is not appropriate for the investigation of a sign or symptom.

- Book online.
- Call 13 20 50.
- Call 13 14 50 for interpreter assistance.
- Find nearest screening location.
- No referral required.
- Group bookings are available.

- Takes 20 minutes.
- All female radiographers.
- Patient consent and details are required.
- Results are provided in approximately two weeks.
- With patient consent, the GP is provided with results.
This video takes women through the screening appointment step by step.

- Most women receive a normal result and return to routine screening (every two years).
- Fewer than 10% of women are recalled to an Assessment Clinic for diagnostic testing.
- Assessment Clinics are a free service.
- Investigations may include:
- Mammography
- Tomosynthesis (3D)
- Ultrasound
- Clinical breast examination
- Needle biopsy
- With patient consent, GPs are provided with results.
- If diagnosed with breast cancer, the patient will be advised to discuss treatment options with their GP and request a referral to a breast specialist.
- Women may resume regular screening with BreastScreen NSW five years post-diagnosis, with a written request from their treating doctor.
- GP follow up: GPs are urged to place a rescreen reminder in their records for the patient’s next mammogram.
What is mammographic density?
- Mammographic density is a term that refers to the relative amount of dense breast tissue (glandular and connective tissue), which appears white on a mammogram, compared with non-dense fatty tissue, which appears dark.
- Mammographic density is commonly referred to as ‘breast density’.
What is the distribution of mammographic density of BreastScreen NSW clients?
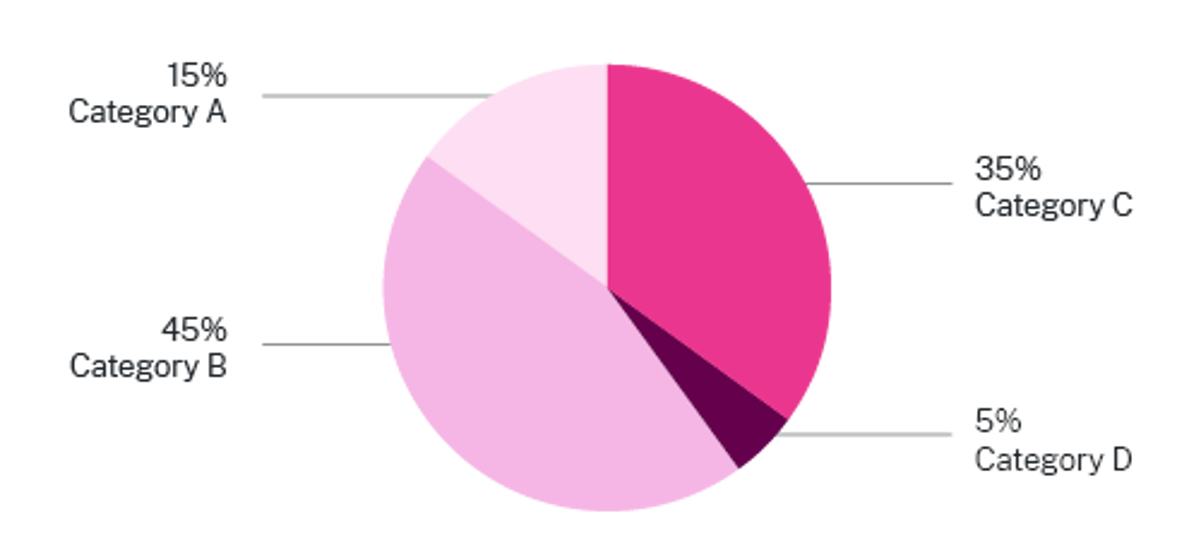
BreastScreen NSW analysis5634 of density distribution by BI-RADS categories using Lunit Insight MMG, 2024, indicates:
- 15% are Category A
- 45% are Category B
- 35% are Category C
- 5% are Category D
How does BreastScreen NSW report mammographic density?
BreastScreen NSW will use software, Lunit Insight MMG, to report mammographic density. This enables clients and their nominated GP to be provided with a BI-RADS density report in the screening results letter. Clients will also receive a breast density factsheet.
The Breast Imaging Reporting and Data System (BI-RADS) is a classification system used by BreastScreen NSW to describe four categories of density:
 Category A
Category A
(least dense)
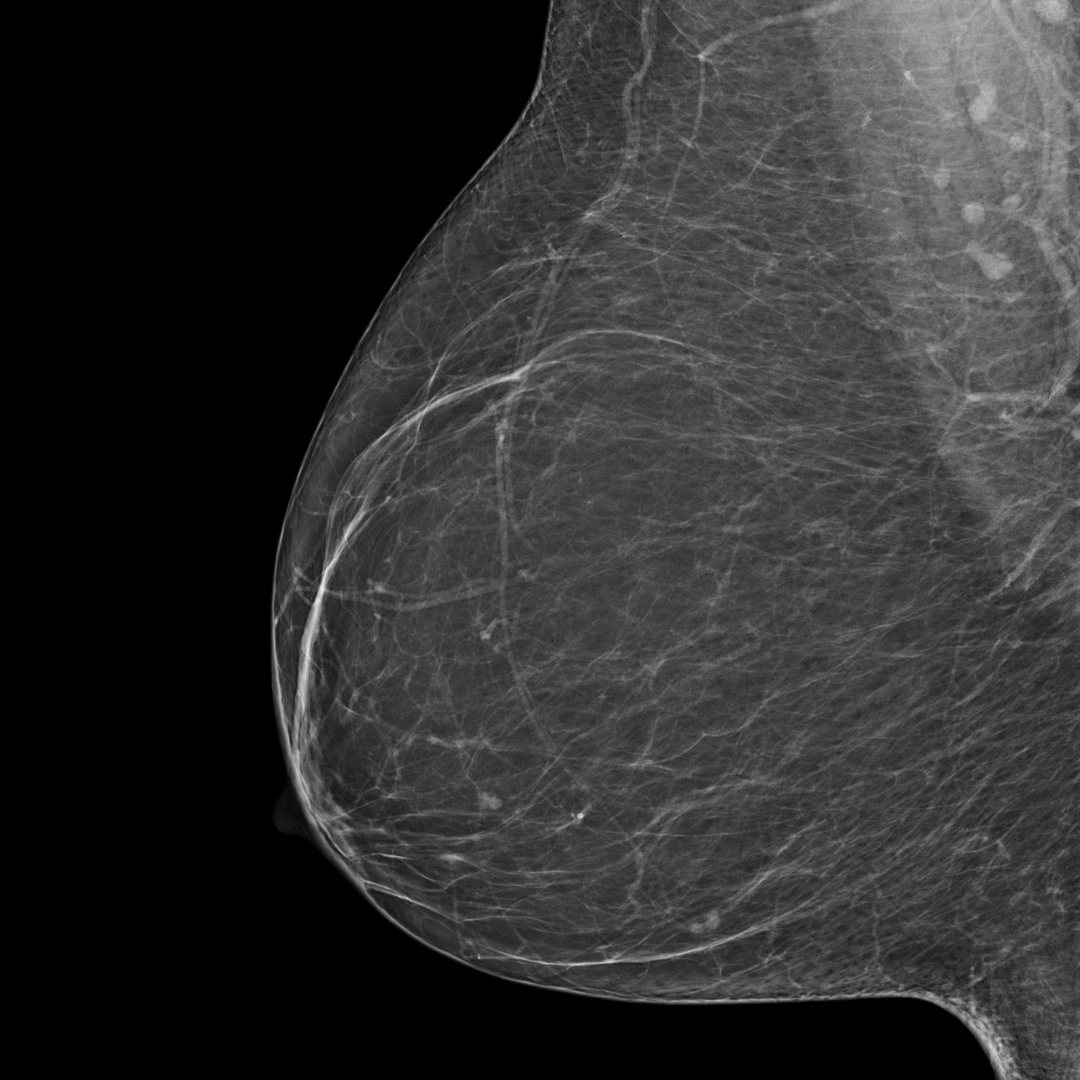
BI-RADS category A:
The breasts are almost entirely fatty. The breast tissue is not dense.
 Category B
Category B
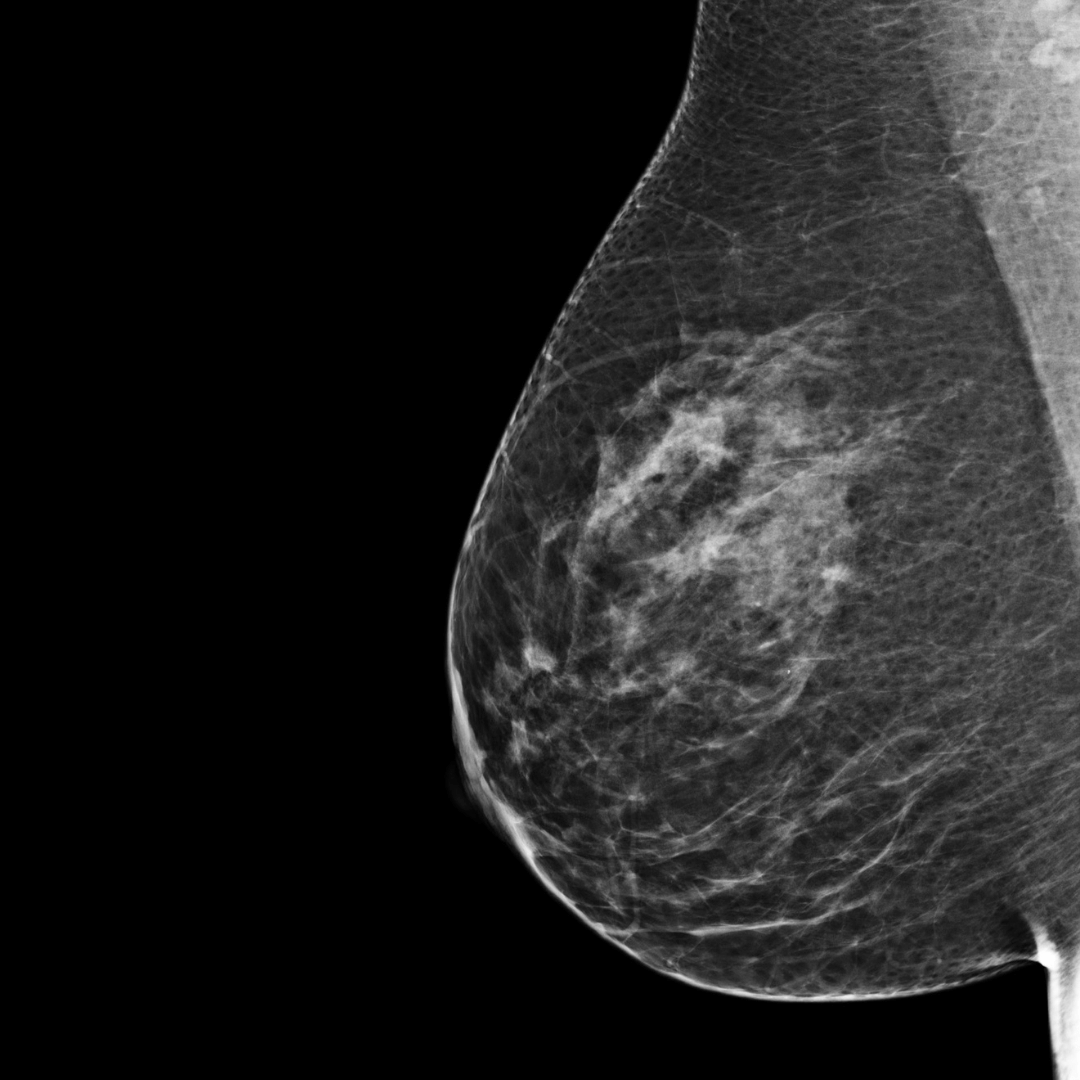
BI-RADS category B:
There are scattered areas of fibroglandular density. The breast tissue is not dense.
 Category C
Category C
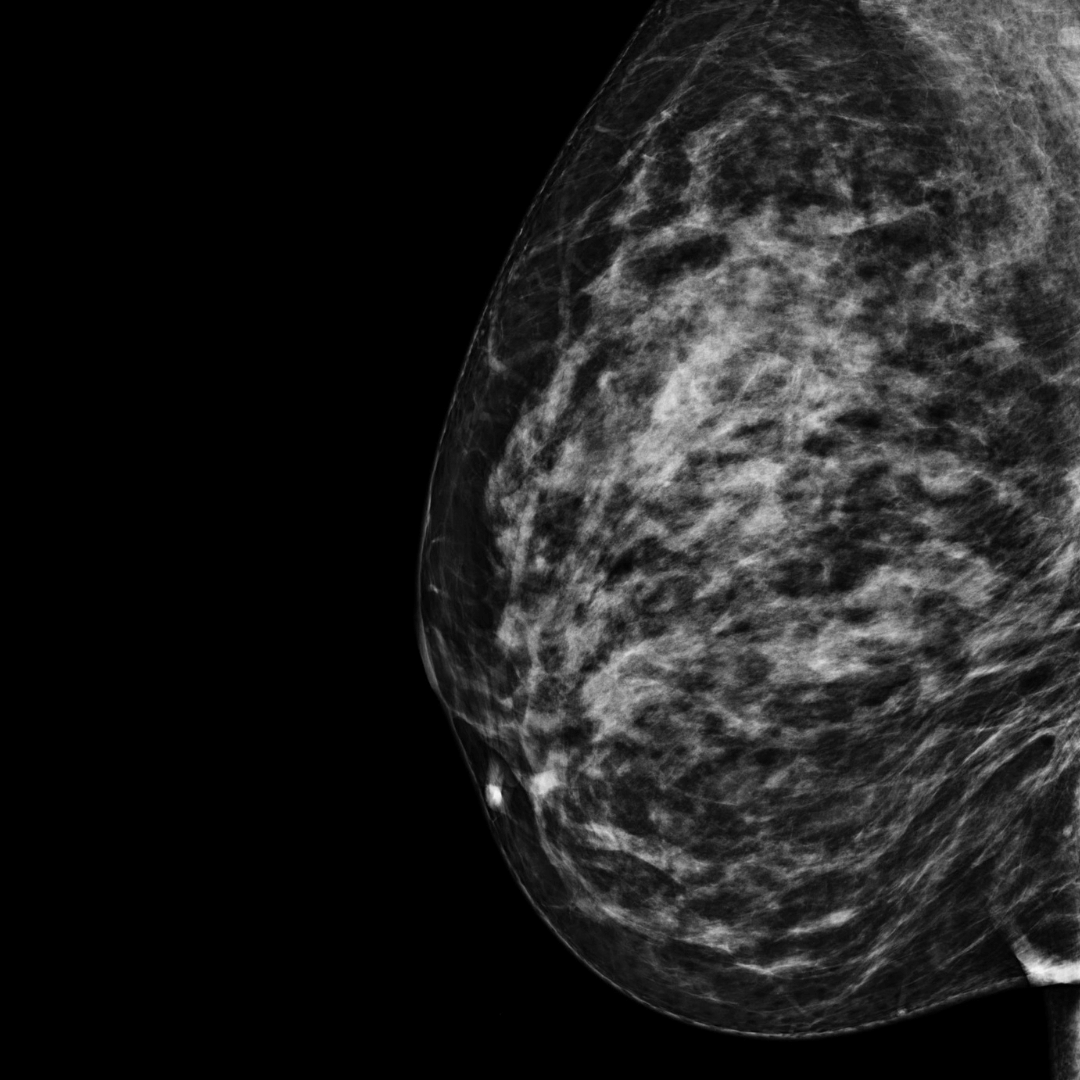
BI-RADS category C:
The breasts are heterogeneously dense. The breast tissue is dense.
 Category D
Category D
(most dense)
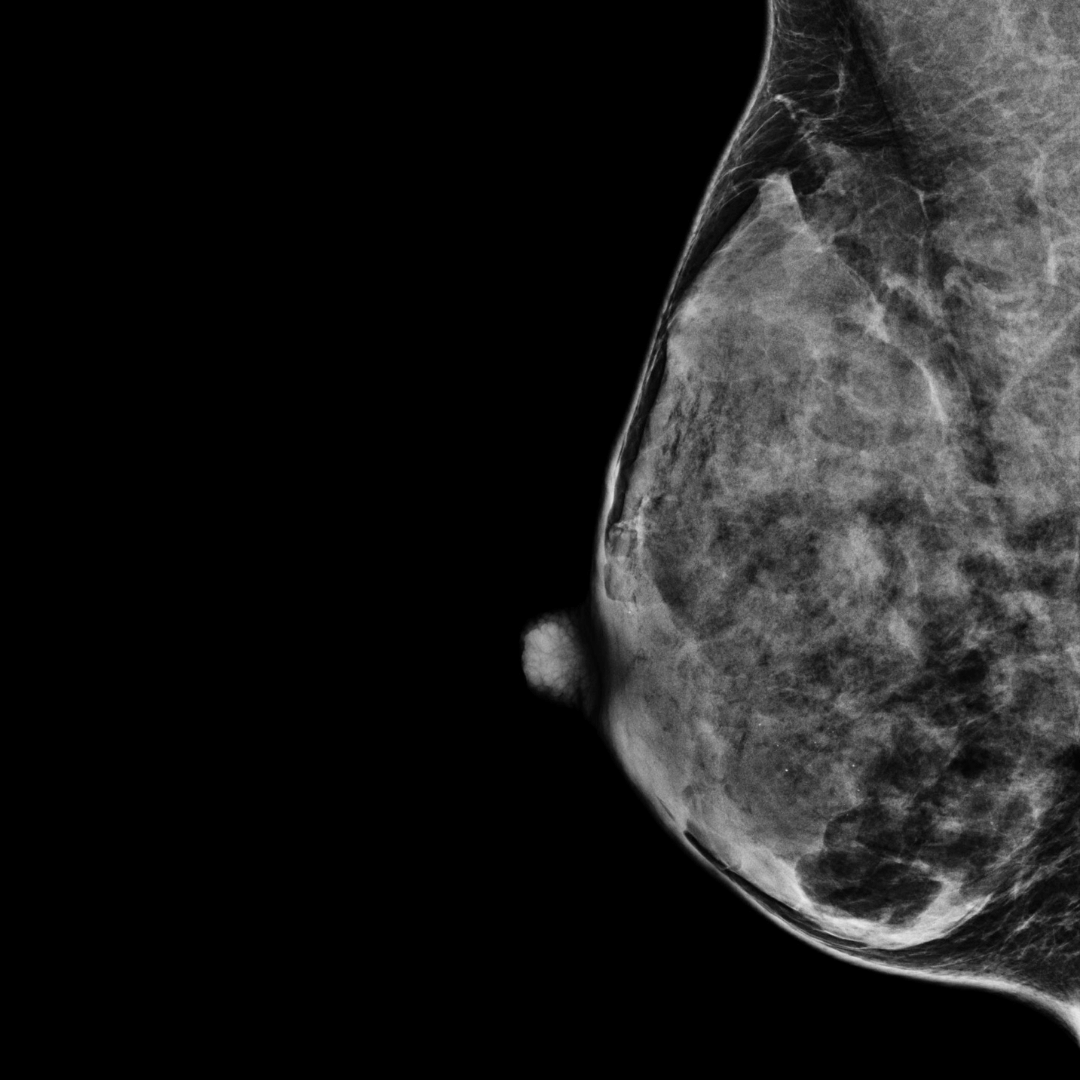
BI-RADS category D:
The breasts are extremely dense.
Mammographic density FAQs
- High mammographic density can lower the sensitivity of mammography as it can obscure or mask small masses which may be cancers. This could result in “underdiagnosis” of breast cancer in women with high breast/mammographic density.
- Studies have shown that Standard 2D mammography has a sensitivity range of 57–71% for extremely dense breasts compared to 81–93% for fibrofatty breasts.
- The sensitivity of a mammography screening program (that is, its ability to correctly identify those with disease, or detection rate), is approximately:
- 90% for women with BI-RADS category A or B
- 84% for those in BIRADS category C
- 64% for those in BI-RADS category D5708
- However, it is important to recognise that irrespective of breast density, mammography is still the best breast cancer screening test in a population-based screening program for asymptomatic women aged 50 to 74 years.
- Increased mammographic density independently increases an individual’s risk of breast cancer and the size of this risk increases with increasing density.
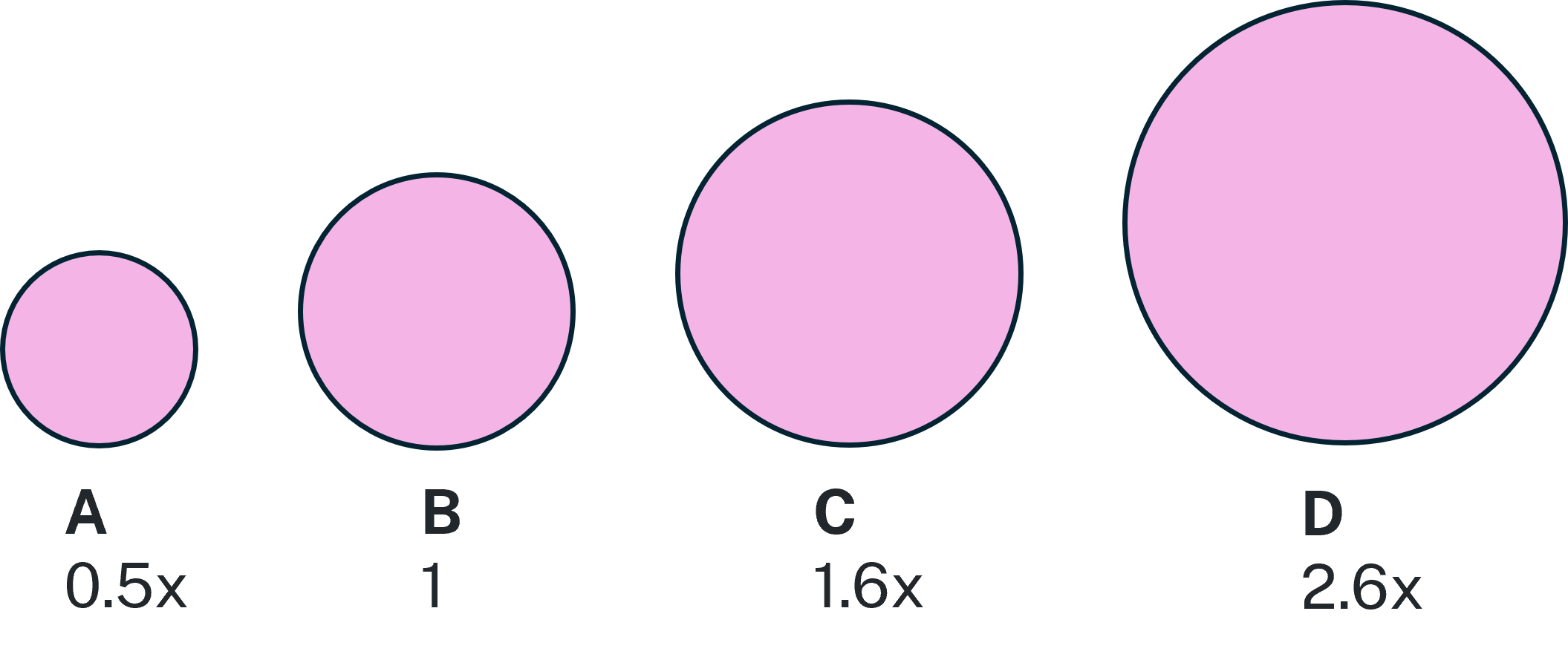
- Image 1. Relative risk associated with density category using the Breast Imaging Reporting and Data System, a classification system used to describe four categories of density:
As a group, women with:
-
- BI-RADS category A have around half the risk for breast cancer than those with BI-RADS category B
- BI-RADS category C have 1.6-fold higher risk than category B
- BI-RADS category D have 2.6-fold higher risk than women with BI-RADS category B.
Image 1. Relative risk associated with density category
- Age is the biggest risk factor for developing breast cancer, with more than 75% of breast cancers occurring in women over 50. There are many other risk factors for breast cancer including non-modifiable risk factors such as age, family history, genetic and reproductive factors and modifiable lifestyle factors, such as being overweight (obesity), being physically inactive and consuming alcohol.
Mammography
- Routine mammography is recommended for women aged 50 – 74 years (40 – 74 years for Aboriginal and Torres Strait Islander women), including those with dense or extremely dense breasts. Even in dense breasts, mammograms detect most breast cancers.
- High breast density alone does not categorise patients as at high risk of breast cancer, as other factors must be considered. Most women with dense breasts and no other risk factors do not require additional screening beyond routine mammography.
- See three patient presentations and approaches in the case studies below.
Risk Assessment Tools
- GPs should consider high breast density in the context of a patient’s overall risk for breast cancer including other risk factors such as age, family history, and genetic variants, and modifiable risk factors. Supporting patients to reduce modifiable risk factors is an important role of GPs.
- Using a validated risk assessment tool can provide the basis for discussions between women and their doctors about their individual breast cancer risk, prevention and screening management.
- iPreventTM Risk AssessmentTool (AUS) developed in Australia, estimates a woman’s breast cancer risk and provides a breast cancer screening and prevention report, including screening recommendations and risk reducing options, that is personalised to that woman.
Access the iPrevent tool here.
iPrevent risk categories below incorporate additional risk factors, including density:
| Average risk | < 1.5 times population risk | Example iPrevent report - Average risk |
| Moderate risk (somewhat increased) | 1.5 to 3 times population risk | |
| High risk (substantially increased) | > 3 times population risk |
iPrevent for Aboriginal and Torres Strait Islander women and other language versions are in development.
-
- CanRisk AssessmentTool (UK) calculates breast and ovarian cancer risks based on an individual’s personal risk factors, cancer family history, genetic testing for high- and moderate-risk genes, polygenic scores and mammographic density. It presents the cancer risks in textual and graphical formats to assist the communication of the results. At present, CanRisk has only been validated for women of European ancestry and is most applicable to European populations.
- Tyrer-Cuzick Risk AssessmentTool (USA) This calculator uses the Tyrer-Cuzick or IBIS v8 risk assessmentmodel and requires a detailed patient family history. Note routine screening protocols vary internationally and may not align with Australian breast screening intervals.
Supplemental screening with medical imaging
- There is no consensus in Australia or internationally, on the optimal pathway for those with increased breast density, in part because what is appropriate for any individual woman will depend on other risk factors, as well as personal circumstances and preferences. See Meta analysis Clinical guidelines for the management of mammographic density: a systematic review of breast screening guidelines worldwide. This review synthesizes the international clinical guidelines and the evidence base for screening and supplemental screening recommendations in women with dense breasts.
- There are currently no randomised control trials that show supplemental screening saves additional lives in asymptomatic women with no other risk factors for breast cancer. However, it is recognised that supplemental screening may lead to additional cancer diagnoses in some women. Currently, supplemental screening is only available outside of the BreastScreen Australia program following consultation and referral by a GP to a diagnostic imaging service. This includes magnetic resonance imaging (MRI), breast ultrasound, digital breast tomosynthesis (DBT) and contrast-enhanced mammography (CEM).
- Evidence is still evolving about the most suitable supplemental screening modality, which can be associated with an increase in false positive results (increase in breast biopsies with benign outcomes), with more follow-up tests and increased costs to patients.
- Medicare rebates for services provided by a private diagnostic imaging service are only available in specific circumstances. For example, a small number of patients who meet the criteria will be able to access an MRI under MBS Item 63464. The criterion that may allow access for a patient with high breast density is a lifetime risk estimation greater than 30% or a 10 year absolute risk estimation greater than 5% using a clinically relevant risk evaluation algorithm. Currently, the accepted algorithm is the Tyrer-Cuzick algorithm version 8 or later.
Preventative Medications
- For patients with increased risk, there are preventative medications available for consideration, following consultation with a breast specialist.
Emerging Technologies
- Research and development in breast cancer detection is ongoing and evolving. Future changes to population and individual breast cancer screening will need to be robust and evidence based.
It’s important for GPs and breast cancer specialists to work with their patient to determine the most suitable management pathway for each individual woman with high breast density. See patient case studies at the bottom of this page.
- There is growing awareness and interest in Australia in mammographic density and its role in breast cancer risk.
- BreastScreen NSW has the capability to report breast density to clients and GPs.
- The Royal Australian and New Zealand College of Radiologists recommends the reporting of breast density in both screening and diagnostic settings be mandated in Australia and New Zealand (2023).
- Reporting of mammographic density enables shared decision making between clients and their doctors.
- Reporting of mammographic density facilitates further research and analysis of mammographic density, its measurement, and clinical implications.
- BreastScreen Australia’s Position Statement on Mammographic Density and Screening 2024, was endorsed by the Australian Government’s Cancer & Population Screening Committee and is pending release in 2025.
Yes. Younger women generally report higher density compared to older women. Mammographic density usually reduces with age, particularly after menopause.
Mammographic density is also influenced by other factors including genetics, Body Mass Index (a lower BMI is associated with higher mammographic density), having had children (may decrease breast density), hormone replacement therapy (may increase mammographic density), and anti-estrogen therapy (may decrease mammographic density).
There will be no change to appointment times or the receiving of results. No additional time, imaging or radiation is required to report mammographic density.
Some women experience heavy and lumpy breasts and this can be normal for them. Mammographic density is not related to how breasts look, feel or their size. It cannot be palpated on examination.
Symptomatic women should be referred to diagnostic breast imaging and/or a breast surgeon. Screening mammography alone is not appropriate for the investigation of a sign or symptom.
In a small number of cases the software cannot determine a reading due to technical reasons. This may be due to the presence of an implantable device.
If the issue does not persist, the patient’s mammographic density will be reported at their next BreastScreen NSW appointment.
It can, depending on the type of implant. Patients are advised to inform our staff when they book if they have implants or have had breast enhancement injections, and our radiographer will discuss this with them at their appointment.
It can, depending on the type of device. Some devices interfere with the software reading and may provide irregular results. Patients are advised to inform our staff when they book if they have a medical device in their chest and our radiographer will discuss this with them at their appointment.
- Breast density can be influenced by hormone treatment.
- Reading of mammograms can be impacted by surgical procedures due to the presence of scar tissue.
BreastScreen NSW recommends transgender clients speak with their specialist doctor if they have questions about their mammographic density.
If available, breast density can be provided on request. Breast density will be reported at each screening episode.
Find out more information:
- Royal Australian & New Zealand College of Radiologists Breast Density Position Statement 2023
- BreastScreen Australia Position Statement on Mammographic Density 2024 - pending release
Case studies5693
These case studies include breast density and characterise patient presentations and approaches:
- Female patient
- Age 54
- BI-RADS category D: The breasts are extremely dense.
- Mother diagnosed with breast cancer when 55
- Overweight
- Smoker
- Discuss the patient's risk factors with them: consider using a tool such as iPrevent.
- Encourage patient to modify lifestyle - diet, exercise, no smoking.
- Discuss supplementary testing with patient.
- Female patient
- Age 63
- BI-RADS category B: There are scattered areas of fibroglandular density. The breast tissue is not dense.
- Two aunts diagnosed with breast cancer in their 60s
- BMI 26
- Drinks 1-2 days/week
- Discuss the patient's risk factors with them: consider using a tool such as iPrevent.
- Encourage patient to modify lifestyle - diet, exercise, no alcohol.
- Encourage patient to stay breast aware and continue to have a regular mammogram.
- Female patient
- Age 72
- BI-RADS category C: The breasts are heterogeneously dense. The breast tissue is dense.
- No family history
- Non-drinker
- Very active
- Discuss the patient's risk factors with them: consider using a tool such as iPrevent.
- Encourage patient to maintain lifestyle
- Unless indicated otherwise by other risk factors, supplementary testing unlikely to be warranted.



